People
We are teachers, leaders, researchers, advisors, business professionals and students. Welcome to Northeastern’s College of Science
Michael Abdelmessih
Jeffrey Agar
News
an robots be used to extract ice on the moon? This NASA research fellow from Northeastern wants to find out
Henry Noyes’ wiring work can be seen all over COBRA, Northeastern University’s award-winning serpentine robot designed to tumble down the deep craters on the moon.
As the electrical lead of the Crater Observing Bio-inspired Rolling Articulator project, Noyes designed the machine’s power system, allowing each of its individual modules to function in harmony.
Noyes, who recently graduated from Northeastern with a bachelor’s degree in mathematics and physics, played an important role in the university’s victory in the 2022 NASA Big Idea Challenge.
Led by Alireza Ramezani, Northeastern assistant professor of electrical and computer engineering, the university team was awarded the Artemis Award for COBRA’s potential to be used as part of the space agency’s missions to set up long-term lunar settlements.
Read more from Northeastern Global News.
Photo by Alyssa Stone/Northeastern University
2024 College of Science Commencement Address by Dean Hazel Sive
Provost Madigan, Dr. Dunsire, honored graduates, honored guests, wonderful faculty and staff: Good day!
I’m Hazel Sive, Dean of the College of Science here at Northeastern University.
What a wonderful celebratory moment this is, the culmination of so much hard work with this well-deserved, important accolade. Warmest congratulations to each of you! Let’s have a round of applause for each graduate! Congratulations, Science Huskies!
Your family, supporters and friends have been along for the journey of your degree! Please join me in thanking them! Congratulations Science Husky families!
Each of you graduating today has been accompanied by your teachers, mentors, and advisors. Please join me in a vote of thanks to everyone responsible for your education!
I told you when you came into this elite University that a degree in science is a stepping-stone to anywhere, and a strong investment in your future. Your training has prepared you to be a science professional, that comes with responsibility to use the training for the good of people, society, the planet and for a sustainable, equitable future. You are a spokesperson and part of the vision for the Good Power of Science.
With your base of key knowledge in science, your problem-solving skills, the confidence you’ve built, your creative, can-do spirit, your ethical and respectful mindset, and your experience as a responsible worker, you are among the most employable people on the planet. Well done!
At this time, I know you’re choosing your next steps, some of you have chosen where you’re going next, others of you are thinking hard. You have great freedom to choose where to put your talent and your time. But the freedom can be a bit unsettling, even scary, I know.
And over and over, many of you ask how you should plan out your life’s career path. I can’t tell you that, because I didn’t have a plan, and you don’t need a plan either.
But I thought I’d tell you a couple of stories that may give you a new angle to think about your future.
To begin with, let’s take a poll. Who of you played make believe when you were a kid? Please raise your hand. Wonderful! Now, who of you still play, in some way? Please raise your hand. Brilliant! You are doing something helpful for your future, and that’s my theme for you today: The Power of Play.
Here’s the first story.
Where I grew up, far away in South Africa, our house had a room we called the porch. It was a regular room with a bed and chest of drawers, except the windows had no glass, only screens. In elementary school, I liked playing in the porch because it was set on the side of the house and was private for out-loud activities.
My favorite game was School where I was the Teacher, and my stuffed animals were the Students. I had a small blackboard taped to a cardboard box, and some white chalk. Even in elementary school, I loved science, and my class studied mathematics – fractions and long division. We grappled with understanding how the seasons worked, we did projects on tea production or how trains ran, and we compared structures of insects across samples collected in the garden.
Now, my dad took a nap in the porch every afternoon. He had epilepsy and had to take medicines to control his seizures, and these made him sleepy. Anyway, in the middle of a lesson one day, my dad came into the porch for his nap. I got up to leave, but he said, “no, it’s fine if you stay and keep playing. Play is very useful, he said, “because it helps you choose what you want to do when you grow up.”
My dad’s words were really important to me, both because they made sense and were encouraging, but also because my dad did not talk very much. The medicines he took in those days dulled him and made it hard for him to put words together. So, these clear sentences stood out for me as something to treasure. I’ve thought about them a lot, and my dad was right, as I’ll tell you.
It turns out that many animal species play, often throughout their lives. For example, when honeybees are given tiny wooden spheres, they push them around, and come back to the activity over and over. Tortoises enthusiastically play ball with one another using their noses.
Many a crow has been seen dropping an object like a stone from a roof to the ground, flying down to pick it up and doing it again and again. And if you love dogs, you will know they’re always ready for a game. The purpose of play is debated by scientists, but the point that so many different animals play suggests that it must have some benefit for each species.
Interestingly, play doesn’t seem to make animals more skilled at specific tasks, or better at solving particular problems. But there is clear data that without play, a part of the brain involved in decision-making, the pre-frontal cortex in mammals, seems to develop less.
Moreover, with play, animals are better able to cope, and experience less stress with unexpected or new experiences they encounter. In fact, play may do exactly what my dad said – give you confidence and brain circuitry that helps you decide how to deal with your future career! My Dad was doubly right – playing helped me decide that I love to teach.
And that’s important for you. All the play you did as a kid and as a Northeastern student has been valuable! The clubs, the hikes, your extracurriculars are a kind of play that has helped you be able to decide what’s next. Every time you’ve practiced an interview in front of your mirror, or tried out a complex conversation before the real thing has set you up to succeed.
Those of you who have explored research, may know that a playful mindset can uncover creative approaches to solving research problems.
And this introduces the second story about the power of play that I want to share with you. Some years ago, a talented PhD student in my group, Laura Lowery, embarked on a new project.
It had to do with the fact that your brain is actually a tube. The nerve cells make the walls of the brain tube, but like all tubes, the inside is a cavity, that is filled with a special fluid. If the cavity of the brain is too large, too small or absent, the brain doesn’t form properly and there can be severe medical consequences.
We decided to ask what is so important about the cavity of the brain tube. We used as a model a small, striped fish, the zebrafish, and Laura looked as the brain formed in the tiny, few mm long, zebrafish larvae. Very helpfully, zebrafish larvae are transparent so you can see right inside the developing brain.
Laura set about taking images through the microscope of the tiny larval brain as it formed and came to show me her first pictures. They were good, but it was difficult to see the cavity of the brain tube distinctly. I told Laura that we needed to be able to see the cavity more clearly and to distinguish this from the surrounding brain tube.
I said to her, “I think you should go and play with various strategies, whatever you want to try, and see what you can come up with”.
Two weeks later, Laura came to see me, a big smile on her face.
She showed me images (here is one of them) of fluorescent bright red brain cavity, standing out with stunning clarity against the surrounding brain tube that she’d labeled in green.
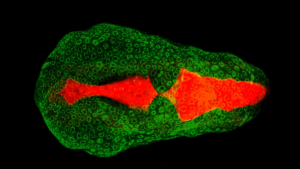
Zebrafish brain tube: green; brain cavity (ventricle): red. Credit: Lowery and Sive, 2005
Wow! Laura had not only identified a red dye that gave this great contrast without hurting the fish, she had pioneered injecting the dye into the brain cavity with a tiny glass needle and injection set up. It was a fantastic moment. Laura said she’d had so much fun doing it!
Laura published the technique she’d invented that is now the standard in the field and used this to identify many genes required for the cavity of the brain tube to form properly and allow optimal brain development. All of those genes are also present in people, and many contribute to brain health.
Dr. Laura Lowery is now a professor at Boston University Medical Center, and I’m immensely proud of her. Laura told me recently that the experience changed her view of science for always, understanding that fun and play could have valuable, important, serious outcomes.
And I think there’s even more. While playing at any age, you’ll often default into what you’re naturally good at. It may be writing, singing, running, dancing, knowing what colors go well together, storytelling, baking, cartooning, organizing events, whatever. When you consider a career path to follow, incorporating something that’s easy for you can be a great way to add a fun and easy dimension to your work, and increase your success at the job.
Overall, playing can develop your ability and confidence to decide what next step to take, play can uncover some of your natural skills, and play will be helpful as you decide where to put your talent and your time!
So, let me circle back to your frequent question of how you should plan your life’s career path? I’ll tell you clearly, for me, there was no plan at all! Rather, starting with a love of science and an interest in teaching, I’ve taken many steps, dozens of steps, along the path of being a student, a professor and now a Dean.
At every step, new opportunities have appeared as if by magic, and I’ve said yes to many of them, even though I’ve often felt underqualified. But, perhaps better positioned by all the playing, I’ve managed to meet each challenge, and you can too.
I’d encourage you to be brave and take each next step, to be open to the pathways that will reveal themselves as you walk along your lives. There are worlds of possibilities in front of you – let each one show itself, and walk right in.
It’s been many decades since my dad’s wise and encouraging words, that playing helps you decide what to be when you’ve grown up. You can play all your life, helping your decision-making process and being better ready to meet exciting, important challenges.
I’m confident that you will find your unique, interesting, useful pathway.
I’m confident that you will take your excellent Northeastern University training in the Good Power of Science, and let it help you move forward.
I’m confident you will be wonderful, empowered, playful Science Huskies forever.
Congratulations once again!
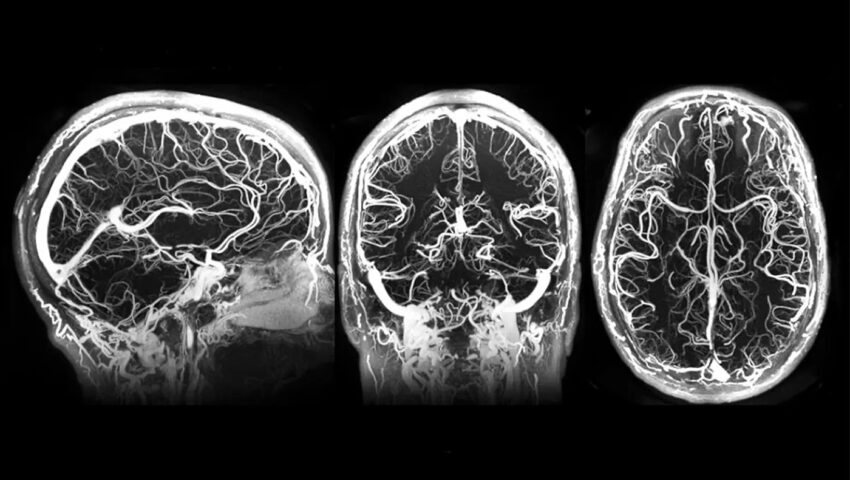
Meet the Innovators: Northeastern grads promise early detection of diseases with breakthrough MRI technology
Codi Gharagouzloo, a physicist and bioengineer, enrolled in the Ph.D. program at Northeastern University in 2011, dreaming of curing cancer.
“I originally came in with this sort of magic bullet idea,” he says. “I thought nanoparticles were just going to be the cure to cancer.”
In the mid-2000s, nanoparticles, a class of tiny materials that cannot be seen with a regular microscope, and nanomedicine, which uses medical intervention at the molecular level, became a highly promising area of research on cancer and cardiovascular diseases.
As a research assistant in the lab of Srinivas Sridhar, director of Nanomedicine Innovation Center at Northeastern and distinguished professor of physics, Gharagouzloo used magnetic resonance imaging, or MRI, to study the use of iron oxide nanoparticles for quantifying the enhanced permeability and retention effect when molecules of certain of certain size can accumulate in tumor tissue.
But he soon realized that nanoparticle drug delivery to cancer would be made successful through specific targeting for specific cancers, driven by discoveries in molecular biology and not physics.
Read more from Northeastern Global News.
Photo courtesy of Codi Gharagouzloo
Embracing the Future: Sacha Sergent’s Commencement Address and Journey with the Northeastern College of Science Class of 2024
Commencement is nearing for the Northeastern College of Science undergraduate class of 2024! This year, at the College of Science graduation, Sacha Sergent will be speaking to her fellow graduates and leaving them with a final hoorah. To get in the excitement of commencement, I interviewed Sacha to learn about her time at Northeastern and what she plans on doing after.
Sacha was born in Paris, France and grew up in Westchester, New York. When she was 8 years old, she toured schools in Boston with her older brother and fell in love with the city.
“I have so many happy memories of us walking around the Faneuil Hall area, taking pictures of all the pumpkins on brownstones, and walking around Kenmore,” she says.
From then on, she knew she wanted to live in Boston.
In high school, Sacha realized she wanted to apply to medical school post-grad but knew there was a chance that she’d change her mind in four years. A school that would give her the opportunity to consider as many options as possible became a priority, and after looking at other schools, it became clear that Northeastern was the place for her.
At Northeastern, Sacha studied Behavioral Neuroscience with her favorite classes being Behavioral Endocrinology; Culture, Tech, and the Future of Health; AI in Health and Wellness; Behavioral Genetics; and Psychopharmology.
Her first co-op was as a medical scribe at South End Community Health Center:
“I loved being a part of the medical team, getting to see doctors go through the medical decision-making process, and getting to interact with patients (especially kiddos!”
Sacha switched it up for her second co-op where she worked in clinical trial development at Prime Medicine in Cambridge. At Prime Medicine, she researched Friedreich’s ataxia, a rare, genetic neurodegenerative disease. She also worked in clinical trial operations and medical writing for their recently FDA cleared Investigational New Drug application for the treatment of Chronic Granulomatous Disease, a rare immunological disease.
Aside from her academic pursuits and professional accomplishments, Sacha was involved in student organizations at Northeastern. Since 2021, Sacha has been a part of CHAARG (Changing Health, Attitudes, and Actions to Recreate Girls), a women’s health and wellness organization that helps students “find their fit” through weekly workouts with local group fitness studios/instructors so members can try different types of movement, as well as socials to build community on campus. She first served as CHAARG’s event coordinator (‘21-’22) then became the club’s president (‘22-’23). This past year, Sacha worked on CHAARG’s national team, managing four executive teams comprised of 35 leaders from other schools around the country. Sacha also taught over 300 group fitness classes at Northeastern!
She has also been involved with NEURONS, Northeastern’s neuroscience interest group. She served as the club’s Public Relations Officer (‘21-’22) and Vice President (‘22-’23. ‘23-’24) where she helped put together last year and this year’s Brain Awareness Weeks, with the themes “Imaging Neuroscience” and “AI in Neuroscience”.
After graduating, Sacha plans on returning to Prime Medicine to continue her work in clinical trial operations and medical writing, leaving behind words of wisdom to her former self: “Follow your passions, lean into your curiosity”.
Congratulations Sacha, and good luck with your future!